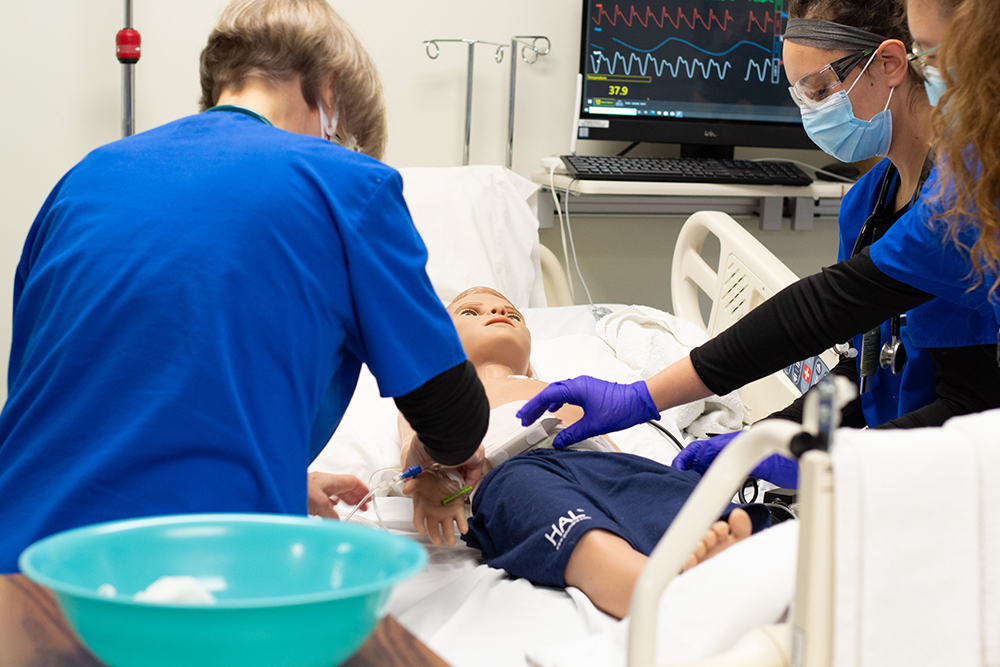
A state-of-the-art pediatric manikin named Floyd arrived at Eastern Mennonite University’s (EMU) campus this fall. The patient care simulator is named after the late alumnus Floyd Zehr ’54, who taught physics and astronomy at Westminster College in Pennsylvania for 35 years. His wife, Pearl, donated the funds for the purchase.

(Courtesy photo)
Investing in the education of future nurses is deeply important to Pearl – she taught nursing at Youngstown State University, and then worked as a substitute school nurse for a few years into her retirement. All of Pearl and Floyd’s children are also connected to his alma mater – David Zehr ’78, Dr. Kenton Zehr ’83, Mary Ann Zehr, an adjunct writing instructor at EMU, and Dr. Bonnie Zehr ’86.
“My children thought that [donation] would be nice,” Pearl said. “I had a wonderful career, and I’m very pleased to have been able to have donated.”
The little Floyd is modeled after a five-year old child, and is “very realistic,” said Professor Audrey Myers. He emits realistic heart and lung sounds that reflect different ailments. He can speak, move his head and eyes, and cry tears. His skin tone changes to mimic conditions like poor oxygenation, jaundice, and fever.
“Students are able to start intravenous access on Floyd, administer medications, and complete many other nursing skills,” Myers explained. “Floyd also is able to respond to interventions that the students carry out, which gives them immediate feedback. It is fun to see how they react to his child-like statements and expressions.”
Myers said that, even when there isn’t a global pandemic going on, “pediatric hospital rotations are extremely difficult to find for nursing students,” so the practice they get working with Floyd is especially valuable.
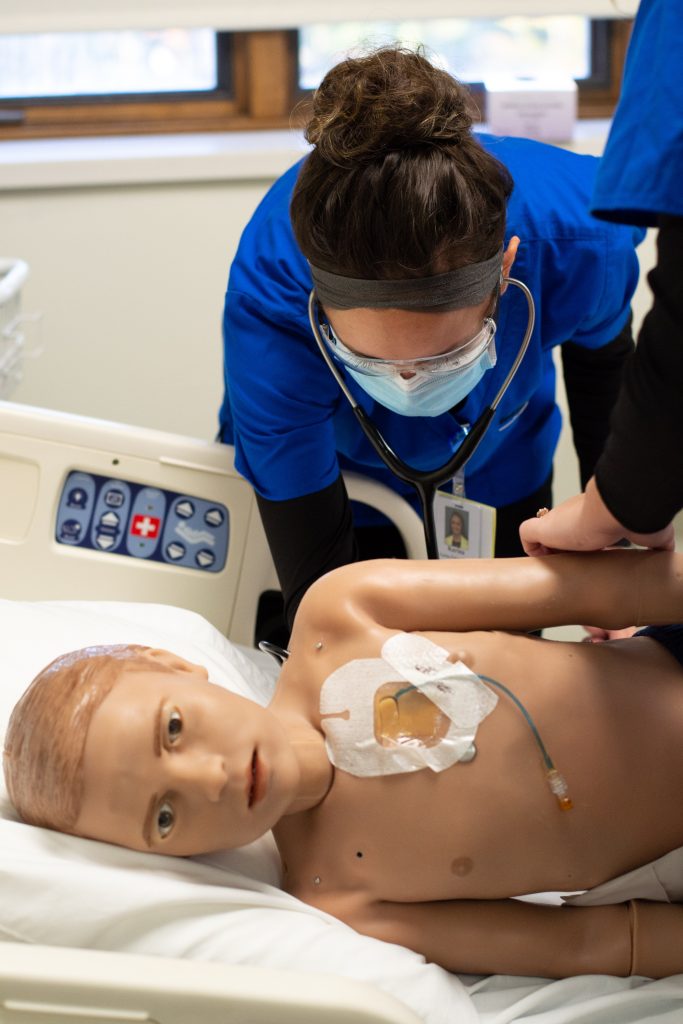
Nursing student Katy Wessel said that, before they had Floyd, they practiced scenarios involving child patients on adult manikins.
“With the pediatric simulator, we can practice complex scenarios on a manikin that has the ability to shiver, become blue or red, have different heart and lung sounds, and generally ‘behave’ more like a child,” Wessel said. “It is very cool!”
Nursing student Karina Pidroutchniak added that “one of the educational benefits is being able to see and hear the normals right next to the abnormals, such as different heart and lung sounds.”
Another benefit of having the manikin is that – unlike with an actual child patient – students can make mistakes and learn from them without dire consequences.
“Of course mistakes are something we cannot have happen in the hospital setting,” Myers said, “but simulation allows us to give our students autonomy to make decisions that may not turn out the way they expect – and I believe this is where some of the best learning occurs.”
Professor Laura Yoder, director of the undergraduate nursing program, said the manikin also allows students to get comfortable with significant clinical situations that are relatively rare, such as hypoglycemic events, allergic reactions, or cardiac arrest.
“By using a simulator, we can give students the practice they need to be able to intervene quickly and effectively in the real clinical environment when these rare situations arise,” Yoder said. “Having high-fidelity simulators in our lab increases the realism of simulation scenarios, which research has shown to increase the confidence and effectiveness of the learner in the real-life situation.”